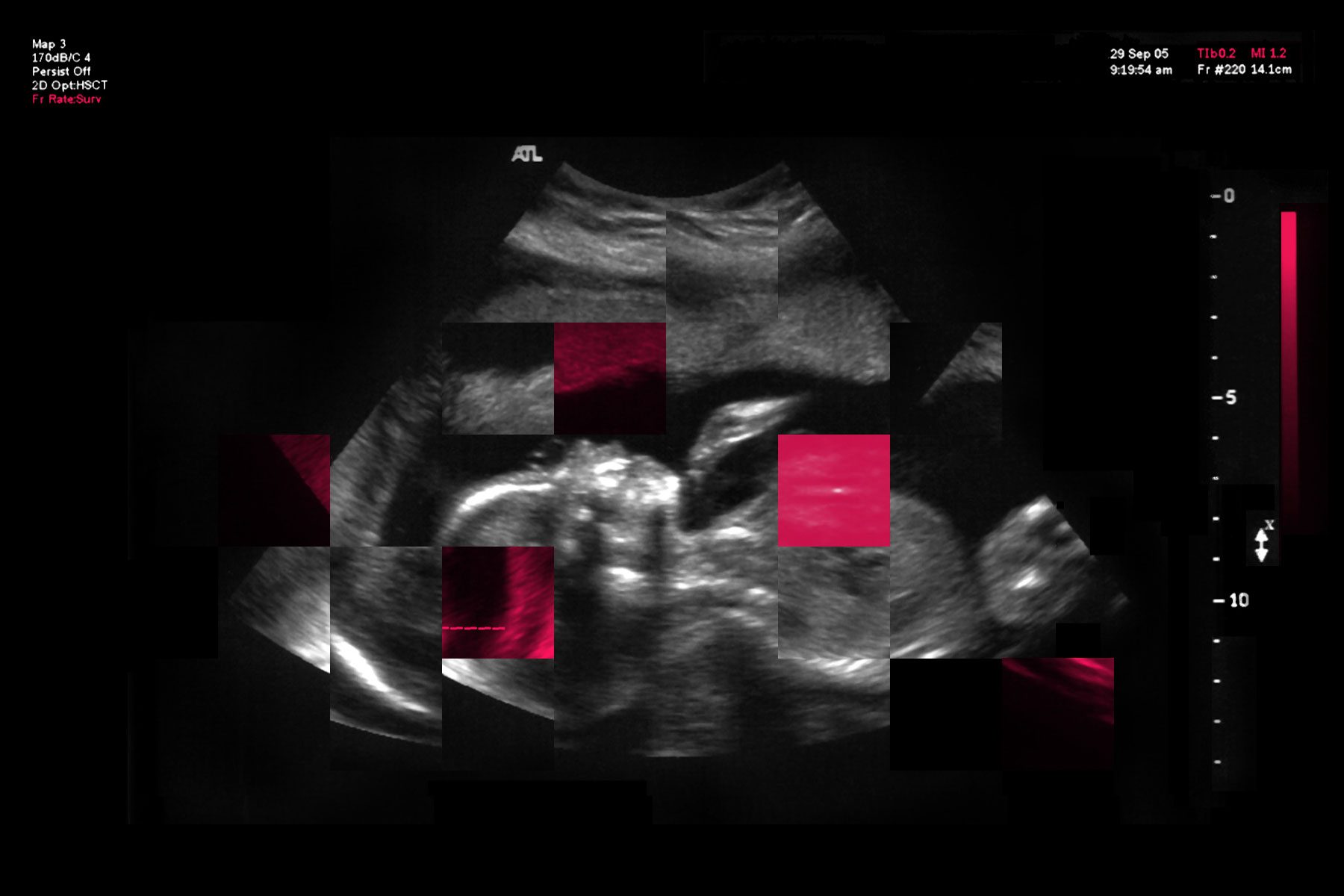
CINCINNATI — Elizabeth D. was 16 weeks pregnant last summer when she went in for an ultrasound and got news that no expecting parent wants to hear.
It had already been a complicated pregnancy. At nine weeks, she woke up in terrible pain that kept getting worse. Her husband took her to the doctor, then to the hospital, where she was rushed into surgery. Doctors found an ovary that had flipped around a fallopian tube, endangering both the pregnancy and her health. They removed it, and her pregnancy continued.
Then, at a scheduled scan seven weeks later, she got even worse news: Her doctor suspected the fetus had anencephaly, a serious birth defect in which the brain and skull don’t fully develop.
“She told me, ‘This is not compatible with life, the baby cannot survive outside of you,’ we’re talking a matter of hours, maybe a day,” Elizabeth said.
Elizabeth’s obstetrician referred her to a neonatal specialist. The details he filled in were not encouraging: If her baby made it to term, then through the birth, he would survive for only a short time. Her options, the doctor said, were to deliver the baby and administer pain medication to keep him as comfortable as possible for his short life, or terminate the pregnancy. Elizabeth thought about the son she was carrying, then the 2-year-old son she already had at home.
“Right away I knew: I can’t carry this to term. I knew I wouldn’t be able to be a good mom to my child. I would be depressed. I knew I couldn’t, my husband agreed,” Elizabeth said.
The next week, the couple drove to one of only a handful of clinics in Ohio that offered surgical abortions. When they pulled in, some of the dozen or so protesters noticed a sticker from a Catholic university on her husband’s car. The protesters yelled that the church didn’t support what they were doing, that there were better options.
She had a surgical abortion at 17 weeks.
“It was so hard not to scream back at them and tell them why we were there,” Elizabeth said. “I wanted them to know — I wanted them to know that this was a wanted baby.”
Elizabeth spoke to The 19th just days after the Supreme Court overturned Roe v. Wade and a six-week abortion ban went into effect in Ohio. We are using her middle name and last initial because Elizabeth is pregnant again — 17 weeks at the time of the interview — and Ohio has a quickly shifting legal landscape when it comes to abortion rights.
The only exception to Ohio’s six-week abortion ban is to protect the life of the gestational parent — a standard medical providers in Ohio and elsewhere have already said is so ill-defined it will lead to delays in critical care. It does not have exemptions for rape, incest or severe fetal abnormalities, including life-threatening conditions like anencephaly. If Elizabeth’s previous pregnancy were today, she would no longer have the option to end it in Ohio.
When the Supreme Court on June 24 issued its decision in Dobbs v. Jackson Women’s Health Organization that overturned Roe, which had protected federal abortion rights for nearly a half century, Elizabeth’s husband texted her at work to tell her the news.
“I had to get off a call, I was crying. We all expected it, but I feel terrible for other women in my situation who now don’t have the option I did. I can’t imagine the mental toll of carrying a child you know is going to die,” she said.
In this new America, the state you live in determines your access to abortion. Medical providers, advocates and liberal lawmakers are pointing out the lesser anticipated impacts of some of these state laws — including situations where fetuses have serious or fatal medical issues.
When Michigan state Sen. Mallory McMorrow, a Democrat, testified before a U.S. House of Representatives oversight hearing last month on the impact of overturning Roe, she focused on a Michigan couple who found out in 2014 at their 20-week appointment that their fetus had severe osteogenesis imperfecta. The baby’s bones were not developing, likely leading to a “very short life, suffering every moment in great pain,” McMorrow said. Now, with Roe gone, McMorrow pointed out that, if courts allow it to take effect, a Michigan law from 1931 criminalizing the provision of abortion would prevent them from seeking in-state care.
About 120,000 pregnancies in the United States each year are affected by fetal anomalies, which are genetic or physical defects of varying severity that can impact pregnancy, delivery and the child’s health, according to the Centers for Disease Control and Prevention. Nearly all of them cannot be diagnosed until well after the gestational cutoffs set by states that have curbed abortion access. And very few have exceptions for the health of the fetus.
Dr. Jessian Munoz, an OB/GYN in San Antonio, Texas, said that in the United States the average patient comes in for the first prenatal visit at about 11 to 12 weeks of pregnancy, and for those who don’t have access to good health insurance or money saved, it can be even later. Over the past decade, there has also been a push to use less invasive or financially onerous prenatal testing procedures, like ordering a blood test instead of an amniocentesis or an ultrasound. It is common, now, for the first scans that might show a serious issue to happen in the second trimester of pregnancy, Munoz said.
“One of the downsides to that is when you’re only doing a blood test, it is primarily looking at Down syndrome,” Munoz said. “Ultrasounds looked at other things too, particularly brain deformities, skeletal deformities, there were some things that you could see earlier that you won’t see now — we’re not even looking.”
All of the nine states that currently ban abortion at all stages of pregnancy — South Dakota, Louisiana, Oklahoma, Texas, Kentucky, Arkansas, Missouri, Mississippi and Alabama — have exceptions to save a gestational parent’s life. Only Louisiana has an exception for “medically futile” pregnancies, but that is not a medical term. Missouri also allows abortions in cases of “medical emergency,” but doctors have said the law is confusing and vague and interferes with patient care.
Tennessee and South Carolina, like Ohio, have six-week abortion bans in place. All three states have exceptions to save a parent’s life but not for rape, incest or fetal abnormalities.
GOP lawmakers in South Carolina have introduced a bill that would ban abortions from conception. An appeals court in Michigan ruled this week that prosecutors could begin enforcing its pre-Roe ban, which criminalizes abortion except to save a parent’s life. In West Virginia, a law banning abortions because of genetic anomalies already took effect. In Indiana, abortions for reasons of sex selection, race or genetic anomalies are already banned and Republican legislators are weighing broader restrictions.
Even though some exceptions for fetal abnormalities exist, Dr. Chloe Zera, an OB/GYN at Beth Israel Deaconess Medical Center in Boston, said doctors struggle to define what a lethal fetal defect is.
“If the sky’s the limit on intervention, and if there are no limits on intervention, then there’s not a whole lot that is purely lethal,” Zera said. “There are a lot of things that are profoundly life-limiting, life-threatening, or are associated with developmental delays, but it’s almost impossible to get definitive. The more common thing is: ‘This is definitely going to mean a lot of medical care, and that medical care might be painful, or that medical care might be unsuccessful.’”
Even if a patient is getting prenatal screenings and scans at every recommended point in pregnancy, many potential issues aren’t diagnosable early on. Most pregnant people have what doctors call the “anatomy scan” around 18 to 22 weeks — parents typically think of this appointment as the one in which they’ll find out the baby’s sex — to look for issues with various fetal organs, including making sure they are inside the body. It cannot be done earlier because for a period in the first trimester, a fetus’ intestines push outside of their body through the umbilical cord, then are pulled back in around 11 to 14 weeks. It isn’t until 15 to 17 weeks that doctors can start to see fetal heart structures clearly. It’s not until 16 to 19 weeks that they can get a good look at the brain, she said.
When doctors see something is wrong, they can rarely confirm that something will be fatal in advance, or advise you on the best next steps, Zera said.
“What we can say is: ‘These are things that are going to mean that your baby has a neurologist, that your baby needs cardiac surgery, that your baby needs dialysis.’ We can give a whole list of likely outcomes based on what we can see on ultrasound. For some families, they’re not a problem. And for some families, they’re an absolute non-starter. And for most families, they don’t know.”
Elizabeth doesn’t talk about her abortion much. Until speaking to The 19th, she’d told only family and smattering of close friends. It seemed too difficult to even revisit in therapy. But when the court overturned Roe, and Ohio’s six-week ban took effect, she wanted to start telling her story.
Elizabeth said she isn’t someone who ever thought they would have “abortion” in their medical file — in fact, she wishes there was a different word to describe her experience, her loss. Yet here she is.
“You think ‘these things don’t happen to us’ and then it’s very eye-opening when it does,” she said.