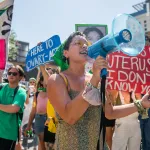The article was published in partnership with USA Today.
It had only been three weeks since Ann Carver and her husband started trying to have a baby, and somehow, she was already pregnant. In the summer of 2022, she’d become a mom.
The couple told everyone they knew, too excited for early pregnancy secrecy and caution. Carver was 26. She felt like there was no reason to worry.
When she was seven weeks pregnant, Carver — The 19th is referring to her by her middle and last name for privacy in sharing her medical history — was on a work trip when she doubled over with cramps. Blood started to leak out of her vagina and she was rushed to the emergency room. Doctors eventually diagnosed her with a subchorionic hematoma, or bleeding between the wall of her uterus and the amniotic sac that surrounded her embryo. Carver’s pregnancy was deemed high-risk — she would need extra medical care and attentive follow-ups. But everyone assured her she would be fine.
At the end of her first trimester, Carver learned she was having a son. She and her husband settled on a name. They set up a nursery and printed invitations for their baby shower. At every check-up, doctors told her things were progressing just as they should.
“We sailed through the rest of my pregnancy. We hit all of our benchmarks,” Carver said. “We had no reason to expect that anything was going to go wrong.”
But things would go wrong, again and again. Carver would lose not one pregnancy, but two.
About 3.7 million babies are born in the country each year, around half of which are considered the result of planned pregnancies. But those numbers tell only part of the story — the version that ends in a nursery, in baby names, in onesies and birthday parties.
Less discussed are the pregnancies with very different outcomes: Miscarriages, which occur in up to 1 in 3 pregnancies, are often the most commonly discussed form of pregnancy loss. But for many people, miscarriage isn’t the only nonviable pregnancy. There are situations that threaten the health of pregnant people themselves, such as ectopic pregnancies, a life-threatening condition. There are the pregnancies terminated because of medical complications and health concerns that are often only discovered in the second trimester. Stillbirths represent yet another form of loss, defined by the Centers for Disease Control and Prevention as when a fetus dies after 20 weeks of pregnancy.
And the standard medical treatment for any of these conditions often relies on access to abortion.

Abortion bans have jeopardized access to care for miscarriages and other pregnancy-related complications. The stakes associated with losing a pregnancy are high, with increased medical and legal risks, especially in the 14 states where abortion is now almost entirely outlawed and the two more that ban the procedure for people past six weeks of pregnancy — including Georgia, Carver’s home state.
Trying again after losing a pregnancy has never been easy. Now, for people like Carver, it feels potentially dangerous.
“It feels like I know all of the ways that things could go wrong,” Carver said. “There’s a burden — I feel anger, if I think about it.”
Pregnancy loss in America has long been a lonely experience.
A 2015 study found that a majority of American adults believed that miscarriage occurred in 5 percent of pregnancies or fewer. About 47 percent of people who had a miscarriage said they felt guilty; 41 percent said they felt like they had done something wrong. It’s a consistent theme across different kinds of pregnancy loss; a smaller study also published that year found that Americans who terminated their pregnancies because of fetal anomalies often blamed themselves for their diagnoses, and reported social isolation because of the stigma surrounding abortion.
In the United States, at least, the silence could be changing after the Supreme Court’s decision in Dobbs v. Jackson Women’s Health Organization, which gutted federal abortion protections. The impact has forced conversations about pregnancy loss into the open.
“People didn’t talk about abortion or miscarriage or medically complicated pregnancy,” said Greer Donley, an associate professor of law at the University of Pittsburgh who studies abortion and pregnancy loss. “The thing with Dobbs is — in my opinion one silver lining — is that people are talking about this a lot more.”
It was the end of January 2022 when Carver, 17 weeks pregnant, went in for her anatomy scan.
Everything with the fetus looked fine, just as it had at every visit before. Then suddenly, the ultrasound technician stopped talking, dropped her wand and left the room.
“What’s wrong?” Carver remembered asking. She was completely alone in the exam room; her husband had come along for the visit, but COVID-19 protocols had forced him to wait in the car.
She couldn’t yet fathom just how drastically her pregnancy was about to turn.
The technician brought back a physician — not the doctor she normally saw, but the first one she could find. He broke the news: Carver’s son had a congenital heart condition known as hypoplastic left heart syndrome. It meant that the left ventricle of his heart hadn’t developed properly. He would need surgery immediately after birth to have even a chance of survival, and subsequent operations after that. Carver had phoned her husband into the visit so he could hear the news along with her.
The doctor did his best to put a positive spin on the diagnosis. This was fixable, he said. She could still have her baby.
Carver and her husband went home in shock. Her father-in-law, a cardiac anesthesiologist familiar with the diagnosis, had a much grimmer analysis of the fetus’ condition. It wasn’t until he started crying on the phone that the couple fully internalized how bleak their chances looked. Carver could stay pregnant, but if she did, they would in all likelihood eventually be forced to watch their child die. Their best option, her father-in-law told them through tears, was to terminate the pregnancy and try again.

It didn’t take long for Carver and her husband to decide he was right. Their own research suggested their son likely wouldn’t make it past his 5th birthday. A cardiologist they eventually spoke with told them that his condition could be cured, but only if he lived long enough to undergo three separate operations — and there was no guarantee he would survive to go through them all — and then be well enough to receive a heart transplant.
“It was like somebody had poured a bucket of ice water,” she said. “Just this steady realization that it’s really, really bad, and it’s not going to get better. And it’s not a mistake. “
It was still months before Roe v. Wade would be overturned, and abortion in Georgia was still legal up until 22 weeks. Carver now had just a few weeks to terminate the pregnancy. She and her husband, while still processing the news, had to find a clinic and a provider who could see them and figure out how they would pay for her procedure, which wasn’t covered by insurance. There was only one clinic in the state that provided abortions past 20 weeks.
The immediate days after the diagnosis felt like a nightmare, the grief paralyzing. Carver, out in the yard with her puppy at 3 a.m., found herself screaming into the dark sky as she processed how unfair it all felt. She spent hours on the couch watching the cartoon ”Bob’s Burgers” while her husband called doctors and clinics to try to set up an abortion appointment.
Carver was 21 weeks along when she finally got her abortion. It was just days after Valentine’s Day, her wedding anniversary. The abortion, including cremation services for their son, had cost the couple about $1,700, which her in-laws gave them. In the weeks after abortion, Carver would wake up hearing what she could swear was the sound of her son crying. As she futilely searched rooms, shaking off sleep, the memory of the loss would sink in again.
Carver felt like she wasn’t fully allowed to grieve publicly. How was she supposed to tell people what had happened to her son? What about those who didn’t understand why, with even a sliver of hope, she would choose to terminate her pregnancy?
The distinction she perceived — the idea that because she had even a nominal choice, some might view her loss as less meaningful, her grief as less potent — is not uncommon.
“There is stigma for both pregnancy loss and abortion, but the abortion stigma is unequivocally worse,” Donley said. “The idea is even when you’re terminating for a completely nonviable fetal anomaly, there’s this idea that a good mother would carry their child through the end — give birth and hold them while they died in their arms. The idea being here you should be so grateful for every second you get with your child who will die.”
Carver knew almost immediately that she wanted to try again, sensing even as she drove home from her abortion that she would soon be ready.

On May 2, 2022, Carver’s phone lit up with a news alert as she shaved her legs in the bathtub. A draft Supreme Court opinion, the one that would eventually overturn Roe had leaked. To Carver, it was obvious what this meant. Georgia would eventually outlaw the kind of care she had received just three months prior. If she did succeed in getting pregnant again — and if things went as drastically wrong as they did last time — what options would she have?
She left the bathroom to find her husband, water pooling on the floor behind her. They had to get pregnant as soon as they could.
“We both had this ‘Oh, shit’ moment, “ Carver said. “There was that feeling of trying to race the clock.”
Without abortion rights protected, the ability to treat pregnancy loss — or any medically complex pregnancy — has become far more volatile, dependent on state laws as well as how individual doctors and hospitals interpret them.
Donley, the Pittsburgh scholar, learned she was pregnant the week before Roe fell. She remembered visiting family on the border of Missouri, where abortion was outlawed, and Kansas, where it was not. Donley was no stranger to loss: She had terminated her first pregnancy, in 2019, because of fetal abnormalities. She lost a subsequent pregnancy to miscarriage.
“I remember feeling palpably afraid,” she said. “There were all these stories about people with ectopic pregnancies, with hospitals saying, ‘We have to wait until your fallopian tube bursts.’”
She worried about becoming one of those cases. So Donley told her parents that if anything went wrong this time — if she experienced a miscarriage, or they discovered that she had an ectopic pregnancy — they had to be sure to take her across the border, making sure she got care at a hospital in Kansas, and one that they knew would provide abortions. Donley ultimately gave birth to a healthy child.
In a survey published this summer from KFF, a nonpartisan health research organization, 2 out of every 5 OB-GYNs in states with an abortion ban said they had faced new constraints in their ability to appropriately care for miscarriage; a similar share reported barriers in treating patients who had experienced “pregnancy-related medical emergencies.” September polling from All in Together, a nonprofit that promotes civic education for American women, found that 1 out of every 3 women between the ages of 18 and 39 knew someone who had chosen not to become pregnant specifically because they were concerned that they could no longer reliably access appropriate medical care if things went wrong.
Access to care varies based on individual doctors’ legal comfort, as well as nuances of the patient’s miscarriage — for instance, whether physicians can still detect fetal cardiac activity, even though it is clear a miscarriage has begun.
Some anti-abortion lawmakers have argued that their bans shouldn’t affect people experiencing a miscarriage or an ectopic pregnancy. But even in states with harsh restrictions, the ability to get appropriate care varies from physician to physician. The KFF survey found that 30 percent of OB-GYNs in states with abortion bans will not under any circumstances even refer patients to another doctor or even a website that could help them terminate a pregnancy, at least in part because of concerns over the legal risks.
“You can’t imagine [another] situation, particularly something that’s time-sensitive — a potential cancer diagnosis, or some other type of conditions that is acute and needs a rapid response — and the doctor says, ‘I can’t help you, and I cant even send you anywhere,’” said Alina Salganicoff, KFF’s senior vice president and director of women’s health policy. “That’s unheard of.”
But with pregnancy loss, she said, that is often the new reality. The consequences of being denied such care can be fatal.
On July 9, 2022 — her son’s due date — Carver got a positive pregnancy test. Just weeks before, the Supreme Court had overturned Roe, and Georgia would soon begin to enforce its six-week ban. That law, which is now in effect, does not provide exceptions for fetal anomalies like Carver experienced, which can only be detected after the six-week deadline.
Where she had once felt excitement, Carver now felt anxiety, even dread. As her pregnancy progressed — as she and her husband learned they were expecting a daughter — the couple couldn’t let themselves start decorating their nursery or think too much about names. It was the only way to steel themselves for the possibility that something could go wrong again.
As her pregnancy progressed without incident, Carver could barely sleep from nerves. Around the end of her first trimester, her doctor recommended she start taking an antidepressant. Even without an abortion ban, Carver would have been nervous, and now she had another layer of fear to navigate. The anxiety manifested into screaming arguments with her husband, typically rare for the couple: What if she needed an emergency abortion? She’d read the stories about people in Texas, where abortion bans had prevented them from accessing life-saving medical care. What if somehow, they learned their daughter couldn’t survive either — and what if this time, she’d be forced to give birth to a child only to watch her die?

She started keeping a list of the states with abortion clinics that provided care past 20 weeks, just in case.
In October 2022, Carver was set for her 16-week visit. The couple had held off on telling too many people about their pregnancy, deciding that if she crossed 17 or 18 weeks without any medical concerns, they’d finally feel secure enough. She scheduled the appointment for a Monday. It was one of the small lessons she’d learned the first time: If you got bad news at a Friday doctor’s visit, you’d have to wait until after the weekend to get it confirmed.
The night before her appointment, Carver started to feel sick again: diarrhea, nausea, a fever. She took Tylenol and tried to hope for the best. They’d just tried a new restaurant recently. Maybe she was experiencing food poisoning. For all of her anxiety leading up to this moment, she couldn’t let herself process the alternative.
The next day, Carver’s husband was allowed in the hospital with her. They watched the ultrasound, waiting — until, once again, the technician abruptly stopped talking.
They knew what that meant.
The technician couldn’t detect any cardiac activity, and a doctor confirmed the news. Sometime in the past week, they’d lost the pregnancy to what the doctors eventually told her was “intrauterine fetal demise.”
It seemed as if this time, Carver’s health care providers immediately understood the severity of her loss. And she was lucky enough to have a medical team that interpreted the state’s abortion law to permit miscarriage management — something she knew wasn’t a guarantee. The doctor offered her medication, which she would use to try to pass the pregnancy at home, or they could keep her at the hospital and induce labor. The other option, the same dilation and curettage procedure Carver had received for her last loss, was technically possible too, the doctor said.
Carver had to wait days before a hospital bed opened up, armed with a checklist of symptoms in case she became septic. Two days after the appointment, she’d begun to experience vaginal bleeding and stomach pains, per medical records she shared with The 19th. The hospital admitted her, and she eventually passed the pregnancy.
Carver’s doctors sent her home with more anti-anxiety medications. They arranged multiple follow-up visits in the weeks to come. “Mentally, I was not OK,” she said. “But they really followed up with us.”
It was hard not to contrast the experience with her first loss — how much more supported she felt this time, despite experiencing losses that felt to her of equal magnitude.

“There’s a sense to which I feel more at peace about my daughter’s death than I do about my son’s. And I feel like it’s because I got more structured care,” she said. “There’s such a stark difference in how we were treated, and the care that I received.”
Carver took several months off before starting to try again to conceive. Both she and her husband, she said, needed to be in a place where they woke up each morning feeling something other than grief, where they could talk about their losses without one of them starting to cry. And even when she finally got a positive test, in July 2023 — the third time in less than two years — it remained difficult to process actual joy.
Instead, she said, it still felt like she was waiting for the next bad thing to happen. She still is.
Carver is due March 17, 2024. It’s a date that was already seared into her memory — a year to the day after when she expected to give birth to her daughter.