Almost 20 years ago, Italy tested what it would look like if embryos were given the same rights as a living person. The country put stringent limits on in vitro fertilization treatments (IVF), banning embryo preservation, limiting the number of embryos created a time to three and mandating that they all be transferred to the uterus.
In the years the law was in place, before it was ultimately repealed in full, more IVF treatments failed, more pregnancies resulted in no live births or more multiple births, and IVF became more difficult to access — and more expensive. Italian patients who could afford it traveled to other countries across Europe to receive treatment. Success rates at IVF clinics dropped, high-risk pregnancies increased and doctors had to risk transferring embryos that could lead to medical complications for the pregnant person. Single parents and many LGBTQ+ parents couldn’t access IVF at all because surrogacy and sperm donation were also banned.
To doctors in the United States, Italy was an extreme example of what could happen if embryos were treated as people, even though in most cases — both in the lab and in nature — a large portion of embryos never become babies. Now, they’re worried that the increased barriers and cost that doctors saw in Italy is a preview of what could happen in the United States.
Any day now, the Supreme Court is likely to overturn its 1973 Roe v. Wade decision, according to a draft of the decision leaked in May, leaving the choice of how to limit abortion access up to states. The impact is expected to trickle down to fertility treatments. States including Louisiana, Nebraska and Oklahoma have tried to pass abortion restrictions that revise the definition of life to begin at fertilization and that limit or ban discarding embryos, creating the standard that led Italy to impose its IVF restrictions in 2004. While those efforts have so far failed, states are expected to try again if Roe is overturned.

Not only could a decision like that impact patients’ health, but it could take a procedure that is already prohibitively expensive for many families and make it even less accessible, reproductive endocrinologists told The 19th.
Already, one cycle of IVF in the United States runs patients about $23,000 on average. Most patients will go through two or more cycles before they have a successful pregnancy, a cost of about $50,000, according to FertilityIQ, which collects IVF cost data.
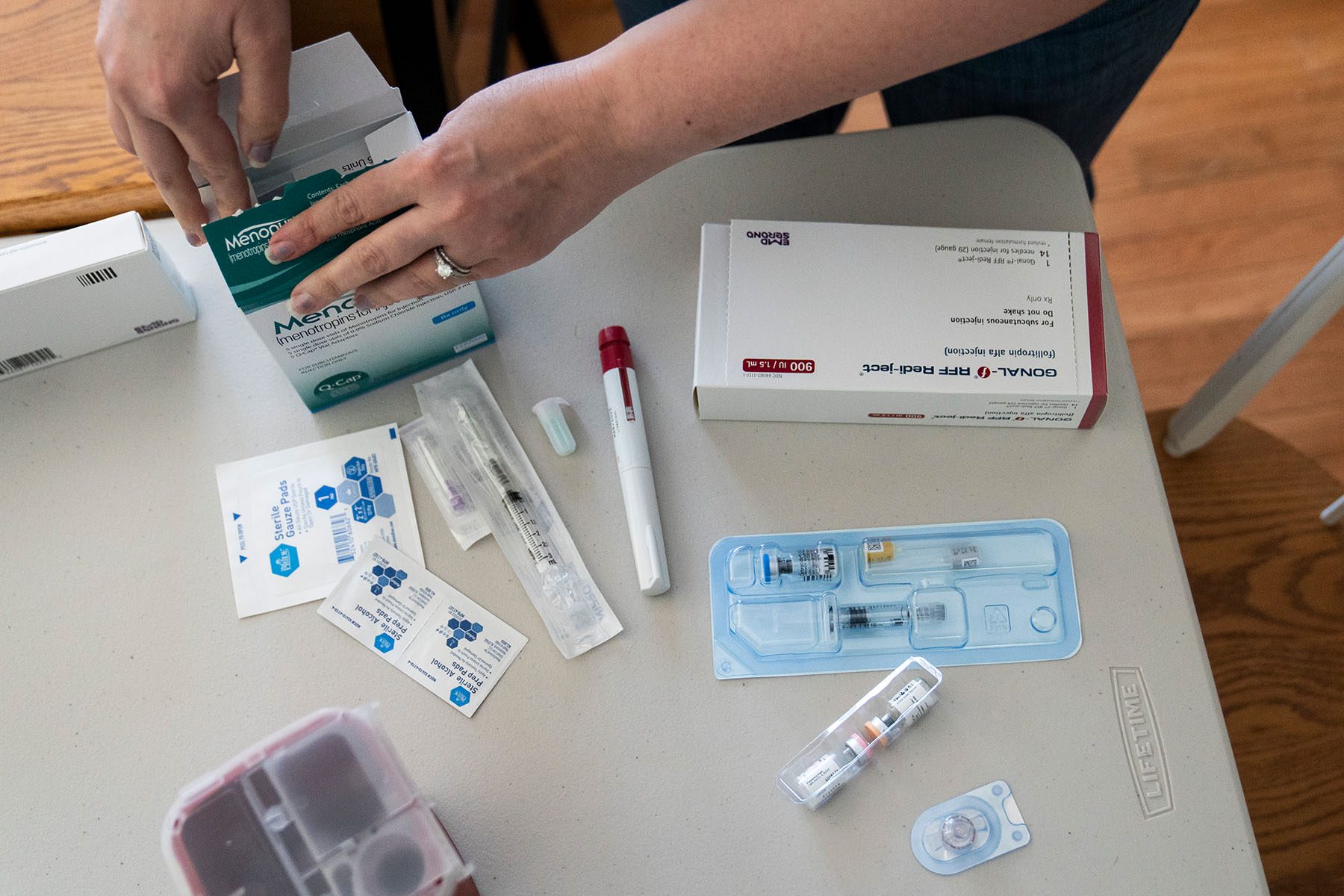
In a typical cycle here, IVF involves retrieving 10 to 15 eggs for fertilization and testing the embryos before choosing typically one for transfer to the uterus. The rest are often frozen, donated or discarded. That approach has led to high success rates for IVF, fewer transfers, and fewer high-risk pregnancies and losses.
Limiting the number of eggs that can be retrieved in a cycle, limiting genetic testing or banning embryo preservation means the likelihood that IVF treatments are successful will decrease. That means patients will have to endure — and pay for — more IVF transfers, and doctors will have to assume potential risks if faced with decisions about eliminating embryos.
-
The Latest:
The issue is also one of racial justice.
“The fertility industry is one where the typical patient is somebody who has money, typically White, a little bit older. [It] has already been catering to a narrow population,” said Kimberly Mutcherson, the dean of Rutgers Law School and a reproductive justice scholar. The majority of low-income workers are women of color, and low-income women are also most likely to have Medicaid coverage, which is prohibited from covering abortion care and does not cover IVF. Mutcherson points out that while they won’t pay for IVF, most state Medicaid programs do cover some form of sterilization.
According to a survey of nearly 1,500 fertility patients published in 2020, more than 75 percent of IVF patients are White and more than 80 percent have annual household incomes higher than $100,000. Black women are the most likely to report facing barriers to fertility treatment, and Black and Latina women traveled twice as far as White and Asian women for treatment.
Low-wage people of color, who already have the least access to fertility care, are the same people who have the least access to abortion care.

That limited access is now under siege on both ends, said reproductive endocrinologists and IVF experts, if treatments become more costly.
Patients with the means to do so may move to states with more expansive laws for IVF, and doctors in states that might restrict IVF will move to states where they can continue to practice, said Dr. Lora Shahine, a reproductive endocrinologist at Pacific NW Fertility in Seattle and host of the Baby or Bust Podcast. That will result in further limiting access to patients, particularly in states in the South where the majority of low-wage women of color are concentrated and where most of these “personhood” bills have been introduced.
Dr. Robert K. Hunter II, the practice director at Kentucky Fertility Institute in Louisville, said the fear of losing his job and having to potentially move to another state is very real for him. Kentucky has tried to pass a personhood bill in the past, and it’s one of 13 states with a “trigger law” that would ban abortion immediately if Roe is overturned.
If doctors are limited in the number of eggs they can fertilize, whether or not they can perform genetic testing or whether they can cryopreserve eggs — the same limitations Italy imposed — that could increase the number of IVF cycles patients have to undergo to have a successful pregnancy, and it can increase risk for doctors, he said.
“The cost of continuing to do business will increase for providers, and that will absolutely get passed down to patients,” Hunter said. “And not to mention if we can’t do genetic testing and cryopreservation — that’s a lot of added cost and disappointment and emotional cost with that, as well.”
Hunter said that if that happened, he would become only one piece in a complex IVF process that could see patients seeking care in multiple states.
“For me to become someone that is just making embryos to ship them to Illinois or wherever the closest women-friendly state is — Is that a sustainable business for me? If I just become a monitoring center for a practice that can still perform IVF for another state? I don’t know that that’s a viable practice model for me,” he said. “I don’t know what is coming down the pike. I will certainly do my best to fight for my patients, but at the same time, in all my years of medical school, residency training, fellowship training, I never thought I’d be affected. That wasn’t part of the gig.”
IVF is still protected, doctors stressed, but they have also started to think about what could happen in a world where it’s not.

In Nebraska, Dr. Stephanie Gustin knows it could become a reality. In April, the state tried to pass an abortion bill that redefined life as beginning at fertilization. It lost by two votes. Republican Gov. Pete Ricketts has indicated that if Roe v. Wade is overturned, he will call a special session this summer to reintroduce the legislation. Gustin is part of a coalition of doctors working to inform legislators about the implications such a bill would have for fertility care.
Gustin, who is the medical director of the Heartland Center for Reproductive Medicine in Omaha, one of only two fertility clinics in the state, is conflicted about what to do if it passes.
“I made this promise to do no harm. … Why would I provide my patient with substandard care that, if they could drive to Colorado or Minnesota they could get the standard care of IVF, just to keep my business alive? I wouldn’t be able to sleep at night,” Gustin said. “The problem is that by not having a fertility clinic here, there will be many people who can’t seek IVF care, period. Those people may be like, ‘We would rather have something than nothing.’” She hasn’t yet figured out how she would navigate that.
Programs that provide grants and loans to families seeking IVF treatment are also teasing out how it could impact them and the people they serve. Many of those programs were born of former IVF patients who have faced the challenges of cost firsthand.
Teresa Barbosa, the CEO of Gift of Parenthood, a program that awards quarterly IVF grants to families in financial need, said she created the program in 2019 after spending more than $60,000 — her life savings — on ultimately unsuccessful IVF treatments.
Gift of Parenthood awards grants as high as $20,000 four times a year; more than 15 babies have been born as a result of the treatments they helped facilitate. Many of those who come seeking help are women of color, like her, who are running out of options, Barbosa said.
“They don’t have the access — it’s really scary,” she said. Gift of Parenthood this year added a fundraising feature on its site to help families raise funds for their procedures, as well as a response to the degree of need.
She feels in limbo, Barbosa said, facing the possibility that even more people will need help paying for IVF and she will be able to help an even smaller slice.
Fertility loan providers like EggFund, which helps streamline the application process for IVF patients, already makes accessing loans easier for patients through one application that ensures the money goes to them and not a clinic. That could help in the case that a clinic closes in a state with changing IVF laws, said founder Carmela Rea. EggFund also allows participants to apply with other people, including siblings and parents, to help reach the requirements for a loan. But higher IVF costs will likely mean higher loans and more debt.

Rea created EggFund in 2017 after spending $80,000 of her savings on her own IVF treatments.
“I felt it was wrong that only the wealthy could procreate, and I think it’s a human right if you want to have a family to be able to have it and not to have money be the consideration that decides whether you can have a family if you want it or whether you can end a pregnancy if you don’t want it,” Rea said. “It shouldn’t come down to your wealth.”
Already insurance coverage for IVF is limited at best and nonexistent at worst. Few employers cover it, and those that do are typically larger companies that employ higher-paid workers, like major tech companies.
At the Baby Quest Foundation, one of the most well-known IVF grant programs in the country, founder Pamela Hirsch said she is working to get more employers to cover IVF. Hirsch has helped give 200 grants since launching in 2012 after her own daughter underwent four unsuccessful IVF cycles before welcoming two babies via surrogates.
Abortion restrictions could make it less likely for employers to include IVF coverage in their insurance plans, experts said.
“It’s almost like a collision course: Which direction is fertility moving in? More access to care because people will be lucky to have insurance coverage from their work or the whole industry closing down?” Hirsch said.
Currently, New York requires that large-group insurance policies cover three rounds of IVF. That law leaves out Medicaid patients and those who work for employers with fewer than 100 employees, an estimated 2 million New Yorkers, said Risa Levine, an infertility advocate and former member of the board of directors at RESOLVE: The National Infertility Association, who helped pass the legislation in New York.
She spent $270,000 on fertility treatments.
“As a White Jewish woman whose parents wanted her to have a kid, I was able to borrow money from my parents,” Levine said. But, “it absolutely impacted my financial security. It put me in a precarious financial situation.”
Low-income women wouldn’t even have that choice, she said. And insurance providers are going to reflect the new risk brought on by changes that redefine how IVF can be performed.
“What insurance company is going to cover a clinic and a doctor for malpractice or for criminal behavior if they define life as beginning at conception outside of the womb?” Levine said.
For providers, the entire discussion puts into question all the advancements IVF has made scientifically and politically in recent years.
There are numerous questions and few answers. What will happen to the pace of scientific discovery if fertility clinics close and IVF becomes a niche service? What will happen to patients, if companies are less willing to cover IVF and conversations about insurance covering the procedure die out?
“We are so far from one another,” Shahine said, “and I feel like any restrictions are going to make those gains we’ve already made fall backward.”