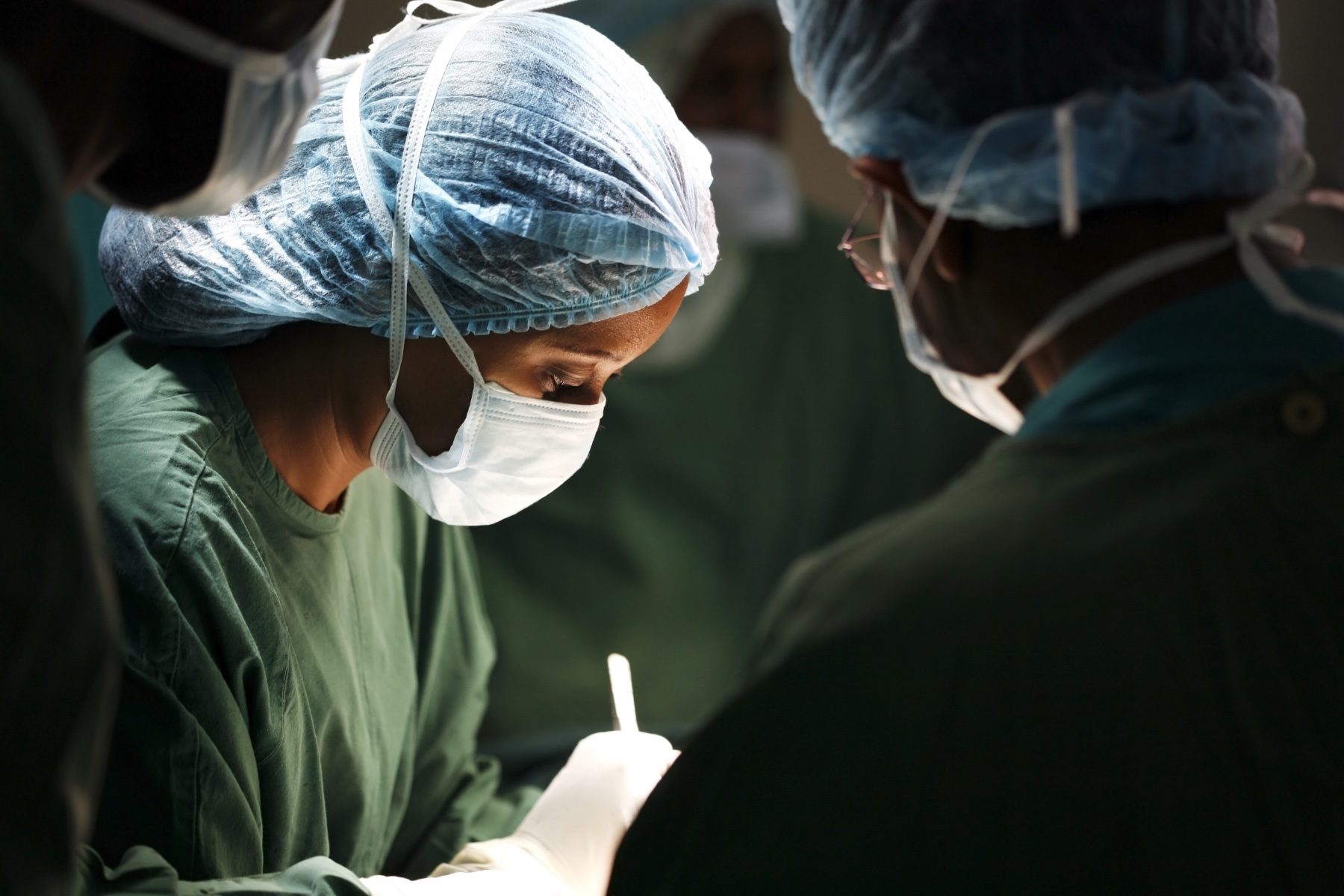
Over the course of their careers, men physicians earn about $2 million more than women physicians, according to a new research paper. And that number likely underestimates the gap.
The paper, published in the journal Health Affairs on Monday, illuminates one of the major barriers toward gender equity in medicine.
“There’s a mountain of empirical and anecdotal evidence that the practice environment is different for female physicians than for male ones,” said Christopher Whaley, a researcher at the RAND Corporation and the paper’s lead author. “We wanted to ask, ‘What is the net impact of the differences across the entire career?’ It’s literally millions of dollars.”
The analysis relies on physician-reported salary data from between 2014 and 2019, looking at self-reported compensation for more than 80,000 doctors. Researchers adjusted the data to account for other factors that could result in salary differences such as choice of medical specialty, years of experience, hours worked, location, practice type and number of patients seen. They then built a model to examine how individual year pay gaps could accumulate over a 40-year career.
The pay gap emerged in every medical specialty, even after controlling for factors like experience and hours worked. In primary care, for instance, men earned about $900,000 more over their careers than did women who worked the exact same job. In surgical specialties, men earned about $2.5 million more.
The $2 million figure stems from direct comparisons between specific types of medicine — analyzing salary gaps between men and women who are surgeons, for instance. But it does not reflect the fact that in general, women are more likely to practice in less lucrative medical professions.
The findings, which are consistent with other research, suggest that gender-based pay gaps emerge early on in doctors’ careers. From the outset, men are paid more than women. Women never catch up. (The data did not account for nonbinary doctors and did not look at race and gender together.)
If anything, the figure likely underestimates the scale of the physician pay gap.
“They’re being pretty generous, relative to what the data actually might show,” said Kathryn Edwards, an economist at the RAND Corporation who studies gender pay gaps but was not involved with this paper.
The 40-year career assumes, for instance, that both men and women work the same number of years in the medical field. But systemic discrimination — combined with responsibilities of parenthood that disproportionately fall on women — could mean that women were more likely to leave the medical field early than men. That would result in even bigger pay inequities.
The researchers acknowledged that likelihood as well.
“If women were more likely to exit active medical practice, as suggested by other studies, our reported results may also underestimate the actual magnitude of the gender income gap,” the paper reads.
Another issue is that of what kind of medicine men versus women typically practice. Primary care doctors and pediatricians, who are predominantly women, are paid less than orthopedic surgeons, for example, who are predominantly men.
“We know that medical students make choices to go into certain specialties depending on how welcoming they think the climate is,” said Diana Lautenberger, the head of the gender equity lab at the Association of American Medical Colleges, who was not involved in the study. “There are studies that show that students are making choices based on gender-biased comments, or racial-biased comments, or what behavior is allowed.”
Medical students and residents often pick their specialties around the age when many are preparing to start families, Whaley noted. If some specialties are not conducive to allowing for child care or parental leave, that could also deter women from entering those fields.
“Easing the transition could help women be more likely to become orthopedic surgeons or specialities that are high-paying,” he added.
Gender-based pay gaps exist in virtually every profession, Edwards noted, and it’s difficult to compare the physician gap to that of other industries. That also means it is harder to devise policy solutions.
“There’s no silver bullet for a physician as a profession. It probably has its own set of demons,” she said. “But it’s still operating in this broader construct of men and women in society.”