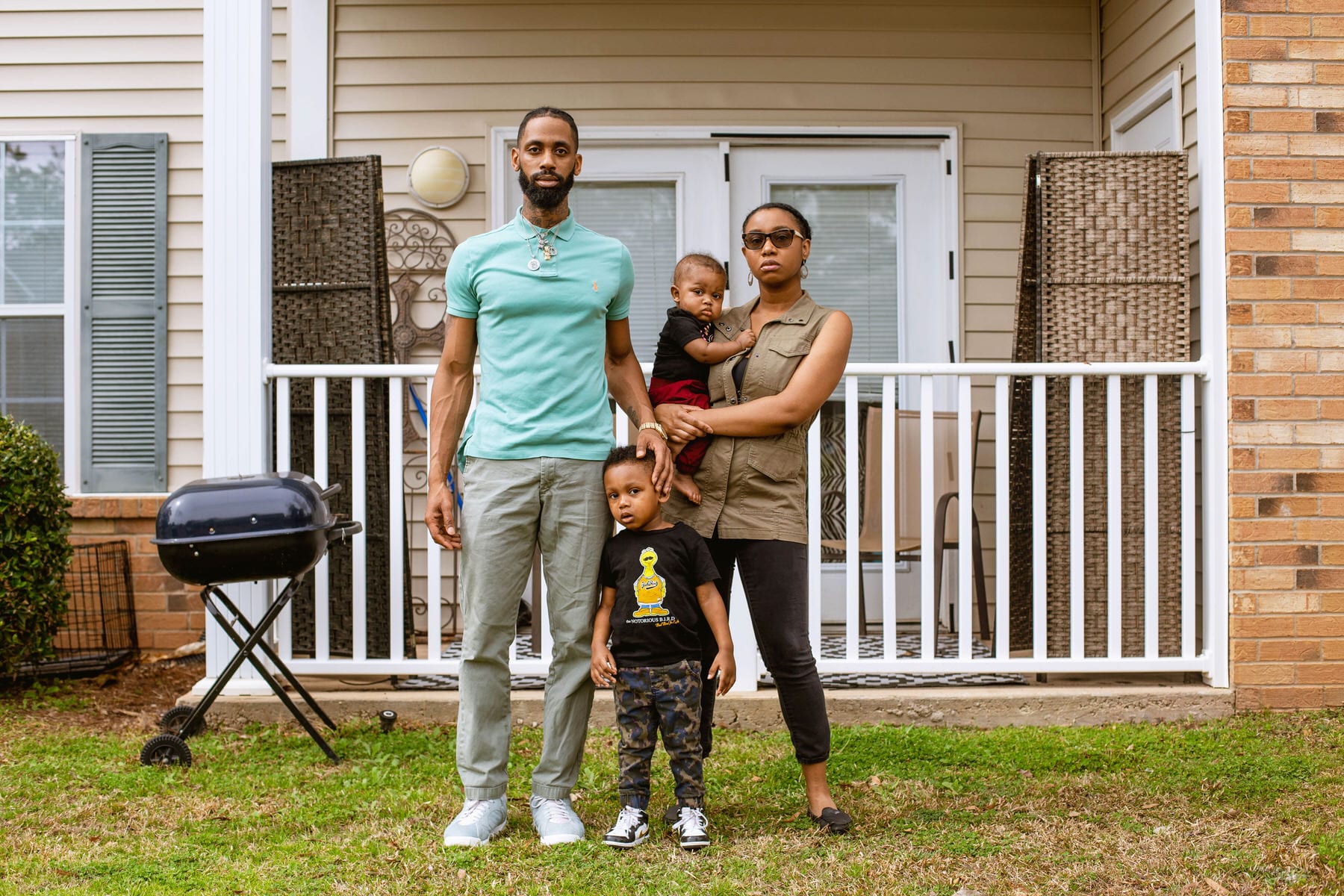When Amira Carson-Carey was in labor last April, she felt so alone. It was two weeks after the Centers for Disease Control and Prevention, changing course, asked the public to mask up, but Amira was bare faced at the University of Mississippi Medical Center (UMCC). Brand new COVID-19 restrictions kept her parents and sister from her.
Doctors detected “non-reassuring fetal heart tones,” and she received an oxygen mask and was anesthetized before undergoing an emergency C-section. Her husband was at the hospital for the birth, but had to go take care of their toddler shortly after. That left Amira alone with her 6-pound newborn, Imani Saadiq Carey.
“Since he got here, it’s been me and him,” said Amira, 33.
At Imani’s first check up, he seemed to be a “healthy 6 days male infant,” as a doctor wrote on his chart. But approximately a week later, Amira noticed something was wrong. Imani wasn’t latching onto her breast, and he had trouble catching his breath. Two days ahead of his two-week checkup in early May, Amira rushed Imani, who seemed increasingly uncomfortable, to the hospital. His heart rate was normal at first, then it nearly doubled. Doctors put an ice pack on Imani’s face to get his heart rate to slow down.
Doctors ordered a COVID-19 test for Imani, which came back negative. But the spiking heart rate and crackling sounds they heard in his lungs signaled a need for a deeper diagnosis. By the afternoon, they identified the problem: Congenitally corrected transposition of the great arteries (CCTGA), a rare heart disease affecting less than 1 percent of infants. In a typical heart, the left ventricle sends blood to the body and the right side pumps to the lungs, just a short distance away. But Imani’s ventricles were reversed, so the right side of his heart, which is not as strong, had to work overtime. He also had Ebstein’s anomaly — which means that one of his valves was not working properly, which can cause leakage, enlargement and heart failure — and was born with a hole in his heart.
While her baby’s heart pulsed arrhythmically, Amira’s sank. “Mom was obviously in shock regarding the new diagnosis,” a pediatric cardiologist at UMMC wrote in Imani’s chart.
Some people live with CCTGA all their lives without knowing it. Others, like Imani, who had trouble breathing and exhibited signs of heart failure, would need surgery once he gained enough weight. Imani would need a double switch surgery, a two part procedure that is ranked in the highest category of complexity by the Society of Thoracic Surgeons (STS), which tracks surgery outcomes.
Amira decided she wanted to move quickly and, in turn, she wanted to see a sense of urgency reflected back from the doctors she would trust to operate on her newborn.
The 19th obtained and reviewed Imani’s 800-page medical records from his time in UMMC’s care. On the same day doctors diagnosed Imani with a congenital heart disease, a pediatric resident — one of several doctors in training who evaluated Imani immediately after his diagnosis — described the infant as “well-developed,” “not ill-appearing.” His discharge papers, also written by a pediatric resident, had similar phrasing: “well-nourished and in no distress.”
Amira wasn’t so sure.
“He looks like he’s doing fine, but his heart is telling us something different,” Amira told The 19th later.
After two days of testing, prodding and monitoring the 3-week-old’s reaction to various medications to regulate his heartbeat, Imani had to receive another ice treatment to his face as his heart rate spiked. The next day, records show, doctors transferred him from the pediatric intensive care unit to the pediatric cardiology unit, and started making a plan to discharge Imani, whom they described as “largely asymptomatic.” “There is no reason to warrant immediate transfer … at this time,” a cardiologist wrote.
UMMC would monitor Imani for one more night, and if he remained stable, he’d leave less than 48 hours after his latest scare. Amira’s concerns only mounted when she was given a stethoscope to “facilitate [heart rate] counting at home since this was of concern to her,” the cardiologist wrote.
She didn’t want to leave so soon after Imani’s heart rate spiked, but she knew she didn’t want her son’s surgery to take place at UMMC — the stethoscope was the last straw. She ultimately received a home heart monitor after “strongly” requesting one, according to hospital records.
Hospital records show that on the same day the UMMC told her that Imani would be discharged, Amira had asked to be transferred to a different facility for a second opinion and requested records be sent to two children’s hospitals in Texas and one in Memphis, all hundreds of miles away. In an email to The 19th, a spokesperson for UMMC said the hospital could perform the procedures Imani needed.
Later, while Imani slept on Amira’s chest in his hospital room, she talked to a social worker, who noted Amira’s “trepidation” with the discharge plan for the next day.
“I had to speak with the social worker and just basically say, ‘Please don’t send me home,’” Amira told The 19th.
What the medical records don’t show is the level of fatigue Amira carried out of that hospital the day after that conversation and into her home in Jackson, Mississippi. She kept replaying scenes of begging doctors to transfer Imani to a bigger hospital, somewhere more accustomed to cardiac surgery on infants. Amira had reached her breaking point. She had more questions than answers. What if Imani’s heart rate spiked again? Would Medicaid cover everything?
And, as a Black woman, she said it felt “triggering” for doctors to continue to refer to Imani’s seemingly healthy demeanor. There is a long documented history of doctors underestimating and even under-treating Black people in pain. She felt heavy, wondering if the weight of generations of racial disparities in health care had descended upon her shoulders.
“There’s a lot of conversations talking around Black women and maternal health and Black children and infants,” Amira said. “I’ve become not just someone who’s looking in, it becomes something that I’m living through.”

Three days after UMMC discharged Imani, Amira rushed him back, reporting that he’d been wheezing. They stayed in the hospital overnight before doctors sent them home again, reminding Amira of signs of distress to look for such as irregular breathing or turning blue. The whole interaction felt very casual, she told The 19th. Amira continued to nurse and monitor Imani as she worked from home as a creative support specialist and waited for a higher-ranked hospital to accept him for surgery.
Then, in late June, Amira’s husband, Demetrius, 35, couldn’t get out of bed after a pickup basketball game; his whole body ached. Within days, they both tested positive for the novel coronavirus. Amira lost her sense of taste and smell, battling flu-like symptoms. Her focus immediately went to Imani. With his heart condition, a COVID-19 infection could be devastating.
Amira said her doctors at UMMC told her to stop breastfeeding and to keep her distance from Imani as much as possible until she tested negative. How, though? she thought. She called back and asked for tips, and she was advised to wear a mask. Imani hesitated to accept bottles, and Amira continued to worry that she had potentially given her son COVID, which the hospital told her he could only be tested for if he started showing symptoms.
Still, she looked toward the future: Imani’s first surgery was scheduled for late July in Texas, about a month out from when Amira first tested positive for COVID.
As her husband remained in Jackson with their 2-year-old, Amira and Imani arrived at Houston’s Memorial Hermann Hospital, her negative COVID-19 test in hand, ahead of the scheduled procedure for Imani’s required pre-surgery COVID test. When nurses returned in full PPE, Amira knew something was wrong. Imani had contracted COVID-19.
“I get really tired,” Amira said. “I tell my support system all the time like I’m tired of fighting — I’m really tired of fighting. I just want it to be over with.”
The more frequently hospitals perform complex heart surgeries, the better the outcome is for patients, experts say. Not all hospitals report their outcomes either on their website or to the STS, a practice that has come under much scrutiny in the last few years. The New York Times uncovered that surgeons at North Carolina’s Children’s Hospital, which is connected to the University of North Carolina, kept operating despite cardiologists expressing concerns about the hospital’s performance: Based on a four year average, in 2017, it had a higher death rate than nearly all of the 82 institutions nationwide that publicly report. A Tampa Bay Times investigation found the Johns Hopkins All Children’s Heart Institute in 2017 had the worst death rate of any Florida pediatric heart program at any point in the past decade.
Dr. Joseph Dearani, chair of cardiovascular surgery at the Mayo Clinic and immediate past president of the Society of Thoracic Surgeons, said that roughly 90 percent of pediatric cardiology programs publicly report their outcomes. UMMC is among those hospitals, and a spokesperson said the hospital has performed 15 arterial switch operations, the first part of the double switch surgery, since 2016. STS data is grouped for multiple years by difficulty of procedures. Dearani said that Amira wouldn’t have been able to see data for the procedures Imani needed in particular, something the STS hopes to change.
“We’re trying to make that better,” Dearani told The 19th. “It’s still problematic because a procedure like this is done so infrequently that it’s really difficult to try to isolate that by itself because it would not take much for things to look very favorable or for things to look really bad.”
What most parents then do, Dearani said, is Google the best surgeons, which is exactly what Amira did after being turned off that UMMC made a plan to discharge her when she expressed that she wanted a second opinion. In an email, a UMMC spokesperson said they “have made, and continue to offer recommendations to other cardiac surgical institutions for second opinions at the request of families.”
Although he had not been her first choice — she preferred top-ranked Texas Children’s — Amira was enthused to find out that Dr. Jorge Salazar of Memorial Hermann had performed Mississippi’s first arterial switch procedure on an infant in 2010, when he was chief of congenital heart surgery at UMMC. Memorial Hermann did not make Salazar available for an interview, but he told UT Health News that after reviewing Imani’s case, “I knew he needed someone to advocate for him.”
As the medical team at Memorial Hermann monitored Imani’s COVID journey, Amira waited for Medicaid to come through. Amira is insured through her job, but to avoid an extra $500 a month in premiums, by her estimate, her kids are enrolled in the Children’s Health Insurance Program through Medicaid, which initially said it would not authorize the procedure out of state. As she appealed to Medicaid multiple times, she wondered if she made the right choice. She thought she was having a healthy baby. Would private insurance have been better? Every day the insurance companies went back and forth with the hospital, Amira said, was a day that Imani’s heart continued to overwork itself.
“Without surgery, there is no survival rate for Imani’s condition,” Salazar told UT Health News.
As Amira waited for a decision, she penned a letter and sent it to various politicians across Mississippi and news outlets, including The 19th. If Medicaid denied all their appeals, she and Imani would have to pack up and go back to Mississippi and back to UMMC, which is connected to the only children’s hospital in the state.
“I am aware that disparities exist in healthcare, and I recognize that in many ways, Imani and I are a part of a statistic that includes Black mothers that have received poor maternal care and, as a result, are facing an uphill battle,” Amira wrote. “I now understand what it means to become a medical advocate for Imani and to harness all the resources available to make sure he has access to the best care possible to him.
“Regardless of my income status, his insurance coverage, or his race, Imani deserves a fighting chance to live a healthy and productive life. He deserves access to the same treatment as a wealthy or white child whose life may be deemed more valuable to the ‘taxpayers of Mississippi.’”
Amira said Salazar told her he was confident the surgeries would improve Imani’s quality of life. “He’ll be able to play sports or be able to do a lot of the things that I would want my son to do, his dad for sure,” Amira said last summer. “Ball is life.”
Dearani said the controversy in heart surgeries like Imani’s is weighing the risk upfront with the fact that, when the surgeries go well, Imani could be able to go to school normally, progress from grade to grade and go to college.
“That is really one of the most important messages with many congenital heart defects, but particularly with a complicated one like this, is that when it works out well, the future is very bright and optimistic for the child and, of course, the family,” Dearani said. “And that is something that should be emphasized.”
On August 1, the same day Amira finished her letter, Imani started testing negative for COVID-19, approximately two weeks after he was diagnosed. Salazar prepared to operate on August 12. The day before the surgery, Imani clung to Amira. It was like he could sense what was about to happen, Amira said. “I’ll probably just hold him for the rest of the day,” she told The 19th via Facetime.
Two hours later, she sent The 19th a text. “Hey! Quick update: They won’t be operating tomorrow,” she wrote. “Medicaid won’t answer the phone for the hospital to confirm coverage.”
It took a couple of days to iron things out with the insurance company, but on August 14, Imani was on the table for about six hours. His chest remained open over the weekend, as doctors made adjustments and monitored him closely. “They’re going to close his chest this afternoon so we’re still in the very EARLY stages of recovery,” Amira texted The 19th.
Amira and Imani didn’t return to Jackson until September, when Imani’s life became a cycle of eating and sleeping — playing when he had the energy. Feeding him was crucial after doctors removed the feeding tube. Imani needed to gain enough weight and strength to undergo the second half of the double switch surgery. He had to eat every three hours, so Amira woke up around the clock with him. She was exhausted.
“What is sleep? Do people need that?” she said.
Outside of hospitals and checkups, there was a lot happening that concerned Amira. Imani had been on earth a little over a month when George Floyd died of asphyxia as a police officer, Derek Chauvin, knelt on his neck for 8 minutes and 46 seconds. Oxygen flowed into Imani’s airways through a tube as protesters around the world hit the streets with “I Can’t Breathe” posters that memorialized some of Floyd’s final words. Amira couldn’t help but notice the parallels.
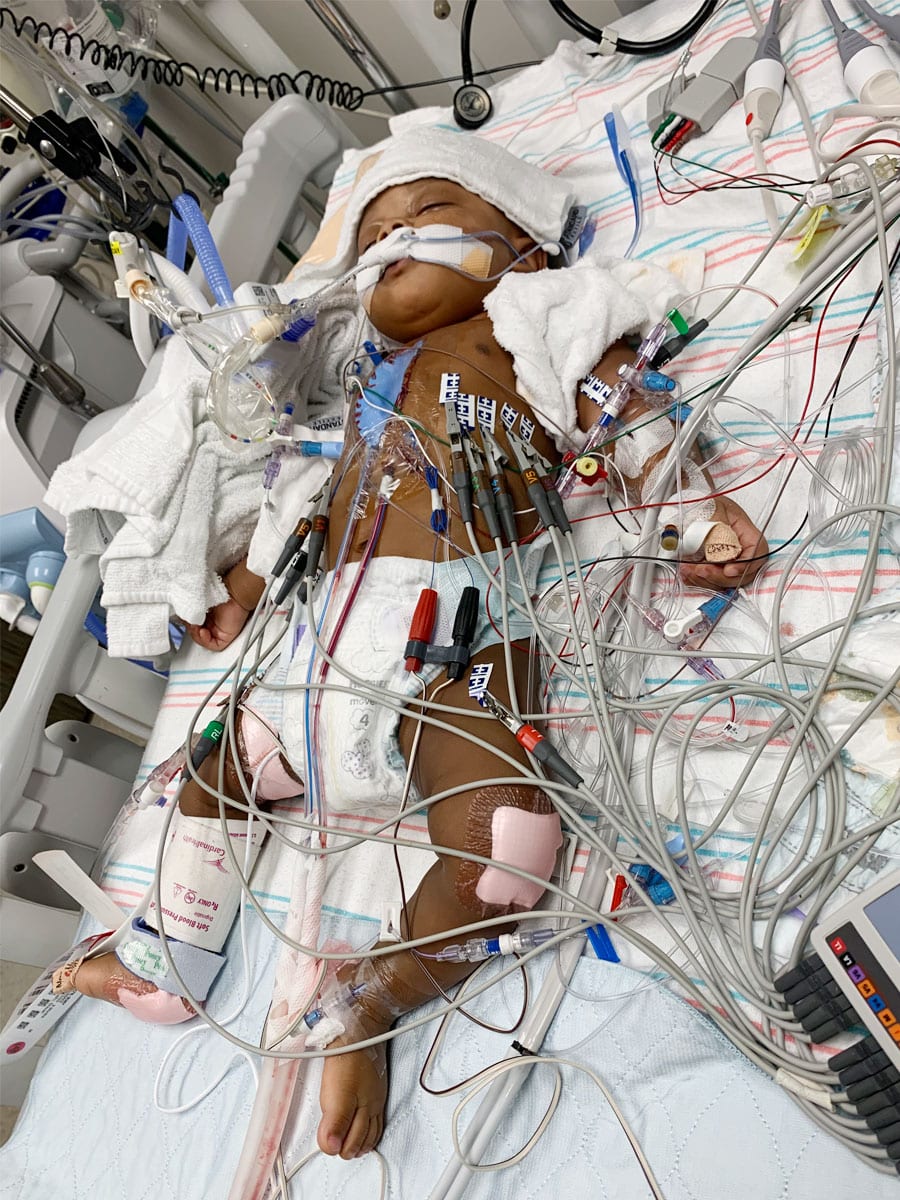
“Those words can mean a lot, not just for what Imani went through — breathing being the only indicator that something was wrong,” Amira said. “But also how systemic racism affects those who are voiceless … Dealing with racism, you don’t know how to speak up, you can’t breathe, you can’t talk, you can’t speak up, you can’t advocate, you just don’t have a voice, you don’t have the words. It’s almost like a two-sided coin: Imani was affected by that, but there are other children and parents who don’t know how to advocate.”
Nakeitra Burse, a public health expert and CEO of Six Dimensions, a public health research company based in Mississippi, wants people to feel empowered when they go to the doctor. There can be such a disconnect, a hierarchy, between the physician and the patient that many are inclined to believe doctors without second guessing them. Having an advocate, whether that be a doula, family member or friend is “critically important,” Burse said, especially for Black people and mothers like Amira. Mississippi has the highest infant mortality rate in a nation where Black women die disproportionately during childbirth, irrespective of income status.
“So it’s not just that they’re not heard about their own body, but it’s that we’re not heard about our children either,” Burse said. “And that adds another layer. At the heart of it is, I can’t call it fracture, but a health care system that just was not built with Black people in mind, and, in many respects, built on the backs of Black people.”
Medical mistrust persists in Black communities, with the Tuskegee syphilis experiment particularly front of mind as the nation rolls out the COVID-19 vaccine, Burse said. But there’s something else — something that just sits in the room, a “silent partner” as Burse described it, when Black folks talk with doctors. It’s the feeling Amira reckoned with as she suspected doctors weren’t really hearing or helping with her concerns about Imani.
“I really believe a lot of it also is just having access,” Burse said. “When you don’t have access to a better provider or to be able to get a second opinion or to be able to shop around, then you are stuck with a potentially biased or racist provider in an already biased and racist system.”
Finances create another barrier to access, Burse emphasized. Mississippi is the poorest state in the nation and it has declined to expand Medicaid year after year. Amira appealed to friends and family for money to offset the cost of Airbnbs, takeout and gas money as she and Imani ventured back and forth from Houston.
“From day one, we were surrounded by advocates, we were surrounded by professionals, we were surrounded by people we could consult,” Amira said. “But there are so many children who don’t have that resource, they don’t have any of that.”
Throughout Imani’s medical journey, Amira started dreaming. She envisioned a new life in Texas, closer to the surgical team. Then her heart landed on New Orleans, so she could be closer to the band she sings for, and the city would be a happy medium between Houston and her family in Jackson. Mississippi needs millennials, she said, but she didn’t want to stay. She put those dreams aside as Imani’s health rapidly declined several months after the surgery.
Imani had a couple of scares where he turned blue and had to return to being on an oxygen tank full time. He had steadily gained weight, hitting 16 or 17 pounds in January, which meant he’d be a good candidate for his final surgery. Amira said Imani had gotten interested in the food she was eating. With doctors approval, she started to give him some, and the weight packed on immediately, creating irresistibly pinchable cheeks.
On February 8, Amira shared a video with The 19th: In it, Imani bounces in his hospital crib, the EKG machine beeping like a metronome. He and Amira had returned to Memorial Hermann — Imani’s weight gain had caused him to outgrow a band Salazar put in place to help with blood flow, pushing his surgery up.
“He was a fully functioning heart!” Amira texted a few days after the surgery. “Post op on the other hand, child, he is OVER IT! Trying to take out his breathing tube, pulling on his cords. And stressing me out lol! Pray for me! Mind you he is on FENTANYL!”
As Amira and Imani prepped for discharge, February’s big freeze took over Texas, cutting off access to power and water to millions as temperatures plummeted. “We didn’t really have water the past two days cause the city was running low,” Amira said via text.
Five days later, they were on the way back to Jackson, which also got hit by winter weather. Large swaths of the city have been without water for nearly a month, and as of this writing, the entire city remains under a boil water notice. Amira said she only got full water pressure restored this week.
Now that Imani is done with surgeries for the foreseeable future, Amira said she can think more clearly, and plan for the future, which, for now, means the family will be staying put. She found a new pediatric cardiologist at UMMC, a Black doctor she trusts a lot. Her hesitancy around moving is primarily rooted in trauma of finding another physician all over again. What would they be like? Would the doctor listen?
“The idea of going through that process all over again frightens me,” Amira said. “While I would absolutely love getting out of Mississippi, I’m really traumatized by that entire experience. Imani having a doctor that I can trust is a huge factor for me.”
Imani’s been going to physical therapy weekly as he continues to recover from surgery. He loves to eat, and fusses whenever Amira is even just slightly late with a bottle or snack, overflowing with laughter soon after he feels full.
When Amira was pregnant with Imani, she went online looking for baby names, African ones in particular. She was making her way through the alphabet, and when she made it to the names beginning with “I,” one jumped out to her: Imani, meaning faith in Swahili.
“It’s almost like foreshadowing — the ups and downs of it all has been very hard for me as far as my faith and the things that I believe in, what I know to be true,” Amira said in an interview. “It’s almost funny how you name your child faith and have to go through the most difficult things that you’ve ever experienced that challenge your faith. It also speaks to the possibilities of what’s on the other side of this.”
Recommended for you
From the Collection