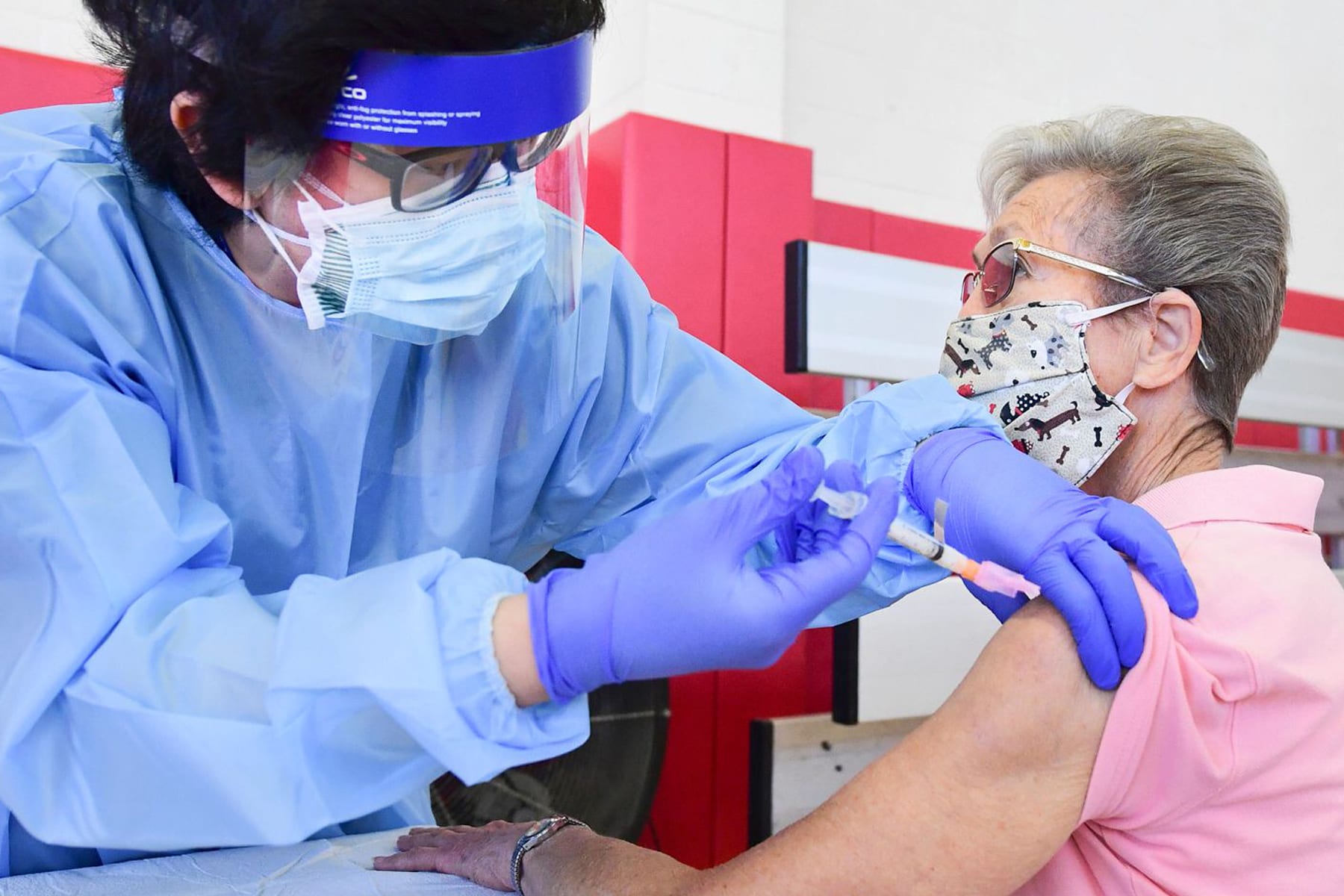
Despite government efforts to vaccinate all Americans — prioritizing the most vulnerable — women older than 65 remain less likely than men of the same age to have gotten a COVID-19 shot, per a new analysis from the Centers for Disease Control and Prevention.
As of April 10, 79.6 percent of men older than 65 had gotten at least one COVID-19 shot, compared to only 77.5 percent of women in that same age bracket — a smaller gender gap than what previous polling had suggested, but still significant.
Overall, the analysis found that by April 10, about 79.1 percent of older Americans had started the vaccination process. (As of May 10, that number is up to 83.7 percent, per CDC data.)
The CDC did not have race or ethnicity data for about 42 percent of the people studied, though what data they did collect found that White seniors were substantially more likely to have gotten a vaccine.
Not every state reported a gender gap: In Montana and New Hampshire, uptake was equal between older men and women, and in South Dakota, a greater percentage of women than men had gotten a shot. In other states, men were more likely to have started the vaccination process, with the biggest differences in Washington, D.C., where the gender gap was about 5 percentage points, and Hawaii, where it fell just short of 4 points.
Counties also varied in terms of vaccine uptake, the researchers noted. Consistently, in areas with low vaccination rates, older adults were less likely to have a computer and more likely to live alone. Poverty rates were higher, and internet access was spottier.
Those are all barriers that particularly affect older women. Women who are 65 and older are more likely than men to live alone, and they more often live in or near the poverty level. That means they are less likely to have people who can help them make or attend vaccination appointments, and more often face financial barriers like paying for transportation or internet.
“They are not only more isolated but may have less access to people in their community or family members who can step in to do all the work that’s required to find a vaccination site to get an appointment,” Tricia Neuman, a senior vice president at the Kaiser Family Foundation, previously told The 19th.
Federal vaccination rates have faltered in the past month, after peaking in April at an average of close to 3.2 million shots per day. Now, the United States is administering closer to an average of 2 million shots per day — a dip that reflects that many of the people who are not yet vaccinated may face more structural challenges in getting to or booking a vaccine appointment, or may require more in-person counseling from their physicians before getting a shot.
The data is the first government analysis to look at age and sex together, and its findings confirm what polling and health equity experts have been suggesting since March. The CDC has not analyzed sex or gender in conjunction with race or ethnicity, raising concerns that experts may not be aware of emerging disparities.
The lack of robust, intersectional data could be a stumbling block in the new phase of vaccination, as policymakers attempt to meet people where they are and determine and overcome their specific reasons for not having gotten a shot.
“You have to understand the people you’re serving, to do what it takes to get them vaccinated, and take the vaccine to them,” Dr. Deepthi Pandita, the chief health information officer at Minnesota-based Hennepin Healthcare, previously told The 19th.