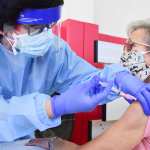
Geneva Eggerson has been eligible for a coronavirus vaccine for months. But she has no idea how to get it, or if she should.
Eggerson’s age, 80, elevates her risk for complications from COVID-19. She has lung conditions that make her even higher-risk. Her home state of Kentucky has been administering shots to adults in her age bracket, 75 and up, since mid-January.
But Eggerson, who lives in Lexington, hasn’t signed up for an appointment. She can’t drive herself to a vaccination site. And, critically, no one has even told her if the vaccine is safe for her, or if getting one is a good idea. (With rare exceptions, the U.S.-authorized COVID-19 vaccines are safe for all adults, including older adults.)
“I want to see my doctor and see what she says — see if it’s all right for me to take it or not,” Eggerson said. “If somebody would talk to me, I might feel a bit better about it.”
The national vaccination effort is, at least theoretically, entering its final stages. The Centers for Disease Control and Prevention estimates that about 55 percent of adults 65 and older are now completely vaccinated against the virus. About 75 percent of people in that age group have gotten at least one shot. President Joe Biden has said that all states must open vaccine eligibility to all people 16 and older by April 19 — and many states have already done so. Meanwhile, drug companies are now moving forward to see if the current vaccines can work on children.
But amid all that progress, women like Eggerson are still being left behind. The Biden administration is calling on seniors to get vaccinated as soon as possible, but as eligibility expands, helping the remaining seniors get shots could become even harder. Early evidence suggests older women appear less likely than older men to have been immunized.
A small handful of states collect gender data when tracking vaccination rates for adults 65 and older, the age group that is by far the most vulnerable to COVID-19. The CDC is currently studying vaccination data to see whether uptake differs for the 65-plus cohort based on gender, but that information won’t be ready until later this month, a spokesperson told The 19th.
But recent polling from the Kaiser Family Foundation (KFF) suggests that, in the 65-plus age bracket, men are significantly more likely than women to have gotten a COVID-19 vaccine. About 70 percent of senior men had gotten at least one shot, compared with only 59 percent of senior women.
The gap, KFF found, is because women are less likely to have even tried to get a shot: About 26 percent of senior women said they had not attempted to book a vaccine appointment, compared with only 17 percent of senior men who said the same. The poll’s findings indicated that older women were more likely to be worried about the vaccine’s safety and effectiveness and that they were less likely to work in jobs that required them to be vaccinated.
But the full picture appears to be more complex. In interviews with The 19th, many women 65 and older pointed to more basic failings. They don’t oppose getting a shot, but they need to hear from their physician that it is safe for them. And so far, nobody has contacted them about getting a vaccine or told them how to navigate signing up for one. All they have been told about is online sign-ups — a barrier for people uncomfortable with the computer or lacking regular internet access.
Problems that impact older people will affect older women more. Women live longer than men, on average. They are more likely to live alone, without people who can help them book an appointment or get to a vaccination site. More than 1 in 5 seniors don’t have steady internet, which increases among adults 85 and older, a group that is majority women. Older women are also more likely than men to live at or near the poverty level, which means they more often face income-related challenges such as getting transportation to a vaccination site or paying for something like at-home internet.
“They are not only more isolated but may have less access to people in their community or family members who can step in to do all the work that’s required to find a vaccination site to get an appointment,” said Tricia Neuman, a senior vice president at KFF who has been studying vaccination for elderly people. “It’s not hard to see how the oldest of old are less connected to sources of information to help them get vaccinated.”
Eggerson lives alone and doesn’t drive — she leaves her house only once a month to get groceries — so she relies on her grandson to take her to medical appointments. He is taking her to the doctor this week, she said, where she hopes to learn if she should take the vaccine. If the answer is yes, she wants to get vaccinated then and there, or at the Walgreens where she picks up her medications.
“They’ll probably have it. When I get my medicine at the Walgreens — I’ll talk to someone,” she said.
The Biden administration has moved to scale up how many vaccines are available in retail pharmacies like Walgreens, which are often more trusted sources of health care for older Americans. Still, getting a shot still requires making an appointment in advance, with availability varying from location to location, day to day.
And those appointments could soon get harder to book.
“Seniors — get vaccinated now,” Biden said in remarks Tuesday, echoing remarks that White House press secretary Jen Psaki made earlier that day .
Immediacy is critical, Psaki told reporters, because as vaccine eligibility opens up to more and more people, the lines will only get longer. Though all adults will be vaccine-eligible by April 19, supply won’t yet have caught up. The Biden administration has ordered enough shots for the entire adult population, but those won’t be fully available until the end of May.
For Debbie Forney, a 66-year-old in Pottsville, Pennsylvania, getting a vaccine took months of waiting and a good amount of luck. Her age group has been vaccine-eligible in her state since mid-January, but she had no way of booking an appointment. As far as Forney could see, everything was online, and she wasn’t comfortable using the computer-based system.
Forney’s daughter works with the state’s senior services and was finally able to find a vaccine phone number, which allowed Forney to set up a time slot. Both she and her husband have now gotten their first shots of the Pfizer two-dose regimen, and she’s passed the number on to other people she knows who are similarly uncomfortable signing up online.
“The only way people are able to enroll in a vaccine is what I did, by word of mouth,” Forney said. “Had I not been told to call that number, I’d still be waiting.”
She worries that it’s a patchwork approach to a systemic issue. In the local newspaper, she constantly sees first-person accounts from older people who aren’t comfortable with a computer and who are writing in seeking help getting a vaccine appointment.
She worries the problem is greater for older women, especially. “So many women I know who are older than me, they’re widows,” she said. Often, they live alone without someone nearby to navigate the Byzantine vaccine registration process.
Forney says more targeted outreach to seniors like her — phone calls, or door-to-door canvassing organized by public health authorities — would help people know where and how to get a vaccine.
But for now? “Everyone is out there on a limb on their own,” she said.
Last week, the Biden administration committed almost $100 million to helping vaccinate adults 65 and older and people with disabilities. The bulk of that money will go toward helping transport people to vaccination sites and to a national vaccine hotline to help people sign up for appointments and get connected to local senior support services.
That could certainly help, but it’s unclear if it will suffice. The government doesn’t actually have solid data breaking down which older people are struggling to get vaccinated, which makes it harder to target solutions or direct information campaigns toward those who need it, Neuman said.
That’s an issue for 82-year-old Darlene Miller. She lives in South Carolina, just outside of Charleston, and hasn’t gotten a vaccine yet. She’s not opposed to getting the vaccine, but she has questions. A polio survivor, she isn’t sure if the shot will be safe for her. (There is no evidence suggesting that COVID-19 vaccines are dangerous for people who have survived polio.) Like Eggerson, she is waiting to hear what her physician thinks, but her next doctors’ visit isn’t until May.
Her area has an ample supply of shots but little outreach. Nobody has called her to talk through her questions about the vaccine, or even to make sure she knows how to get one.
Research suggests that older adults, who generally have insurance through Medicare, are more likely to seek medical answers from their doctors or local pharmacists — and those could be natural hubs for vaccine outreach. The power of a physician’s office appears especially salient for conservatives, who are more likely to be skeptical about taking a vaccine to begin with.
But in much of the country, individual doctors’ offices have taken a relative backseat during vaccine rollout, Neuman noted. Hospitals have played a role in distribution, but more often, shots are mainly organized through health departments, which coordinate directly with pharmacies and vaccination clinics.
“There’s a disconnect in what people think of as their health care system,” Neuman said. “Most people don’t have a personal connection to their county or state public health agency.”
Linda Jewell, a 68-year-old in Rapid City, South Dakota, learned how to get her shot by calling her physician. She got a single-dose Johnson & Johnson vaccine at the end of March. The process was painless, she said.
It’s lucky she called. Jewell had been waiting months longer than she should have, and arguably without any good reason. When she called her doctor, she learned the hospital had mailed her a letter in January, informing her about her vaccine eligibility. Jewell never got it.
She doesn’t use a cell phone, send text messages or spend much time on the internet. The health care system, she said, needs to be doing outreach to people like her, who are high-risk and who would be open to getting a vaccine. That means phone calls to help people set up appointments, and door-to-door visits.
“If they had a small program to call and ask, ‘Have you had your vaccine’ — yes there a lot of people who will be assholes and hang up, but even then, maybe someone will think twice, and say, ‘Maybe I should get it,’” she said.