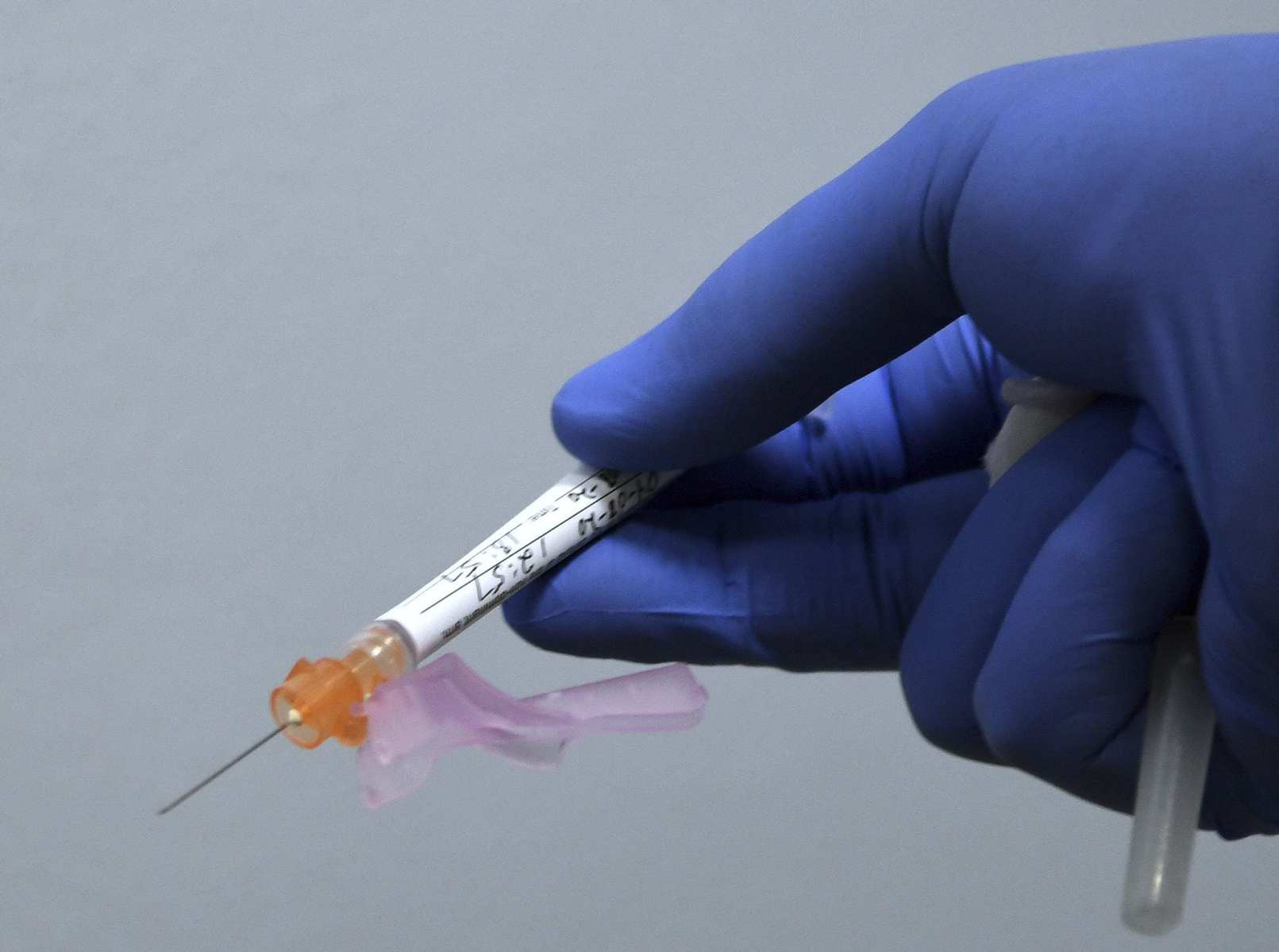
People with controlled HIV are expected to be included in two major federally-backed COVID vaccine trials, a major victory for advocates. The move by drug developers could have far-reaching implications for people who are at heightened risk for both HIV and the novel coronavirus.
The news comes after a vocal campaign by advocacy groups, who argued that excluding people with HIV from trials creates undue risk. But it leaves unsettled a larger debate about who gets to be included in early vaccine tests and who gets to benefit from the COVID immunization that first comes to market.
Massachusetts-based Moderna, which has received close to a $1 billion in federal backing for its COVID-19 vaccine candidate, sparked outcry at the end of July, when it said people with HIV would not be included in its late-stage vaccine trials. Advocates and HIV researchers argued that the science didn’t justify excluding people who are HIV-positive but take medication to suppress the virus. If people with HIV were excluded from vaccine trials, they argued, they might not be immediately eligible for any approved immunization.
“We do want to know whether a vaccine will be helpful, and we want to know what the side effects might be, if different at all, in an HIV population,” said Dr. Karen Tashima, a professor of medicine at Brown University who has researched HIV treatments and leads a local COVID vaccine trial. “My concern is we would have to wait for a trial in the future to vaccinate HIV patients. And we don’t want to wait.”
On Wednesday, Moderna reversed course, putting out a statement that people living with controlled HIV will be included in its late-stage COVID vaccine trial. Moderna cited discussions with the National Institute for Allergy and Infectious Disease (NIAID), which it is partnering with to administer the trial, as well as “the preference of the community to be included.”
The change is not reflected in Moderna’s online filing at ClinicalTrials.gov. Neither Moderna nor NIAID responded to requests for comment.
On Thursday, Pfizer, which has gotten almost $2 billion from the government for its COVID vaccine, but is not using the NIAID-backed COVID-19 Prevention Trials Network, confirmed in a letter to advocates that it is reviewing its policy as well, and is “in the process of amending the [research] protocol” to confirm that people who are positive for HIV can enroll in its late-stage COVID-19 vaccine trial. The final change is pending approval from regulators, Jerica Pitts, a company spokesperson, told The 19th.
“Ensuring that our COVID-19 clinical trials include diverse populations is of primary importance,” wrote William C. Gruber, Pfizer’s senior vice president for Vaccine Clinical Research and Development, in a letter to HIV activists shared with The 19th.
Pfizer and Moderna are the only two companies with government contracts that are currently prepping for late-stage vaccine trials in the United States. (AstraZeneca, which also has received federal funding, is testing its immunization internationally.)
The change likely foreshadows similar policy from other companies. Though the NIAID has not commented on HIV specifically, the co-head of COVPN, which Moderna is leveraging for its vaccine tests, told The 19th that people with “stable underlying medical conditions, including HIV” should be included in late-stage vaccine trials.
“We want these trials to reflect diverse racial/ethnic, geographic and age groups who are at increased risk of SARS-CoV-2 infection,” said Dr. Larry Cohen, a professor at Fred Hutchinson Cancer Research Center and COVPN co-leader.
Historically, people with HIV have often been considered “special populations” whose immune systems could react differently to vaccines. The common argument is that including people with HIV could complicate the dataset or slow down the trial. Already, enrolling people in clinical trials is difficult, and the pandemic nature of COVID-19 makes speed even more important.
But in fact, early data suggests HIV-positive people who are taking regular medication to control the virus are at no greater risk of COVID-19 complications than people who are HIV-negative. Infectious disease researchers reason that those people aren’t “immunocompromised” in a way to justify their exclusion.
“We absolutely positively know if patients who are HIV-positive are well controlled,” said Dr. Geeta Swamy, an OB/GYN and vice president for research at Duke University, citing well-documented cases of people living with the virus for years and even decades.
And from a health disparities standpoint, both companies’ reversal — and the continuing debate over other vaccine candidates — has major implications.
Black cisgender women, per the most recent federal data, are at heightened risk for HIV, making up almost 60 percent of the new cases among women in 2018, even though they represented about 14 percent of the cis-woman population. In 2017, HIV was the eighth most common cause of death for Black cis-women between the ages of 35 and 44. (Black gay and bisexual men account for more HIV diagnoses than any other demographic.)
Meanwhile, COVID-19 has hit Black people harder across genders. Data from the COVID Tracking Project shows that Black people in the United States are dying at more than double the rate of White people from the coronavirus, and at a higher rate than any other racial group. Another study from the University of Pennsylvania found that Black pregnant people were five times as likely as White pregnant people to have been exposed to the coronavirus.
Data from the Williams Institute, which is operated by the University of California, Los Angeles, notes that transgender people are at elevated risk. Of the 1.4 million trans people, 74,800 — or almost 5 percent — were living with HIV in 2016, the most recent year for which statistics are available. Plus, federal data shows that the majority of trans women who are served by the Ryan White HIV / AIDS program are Black. According to a 2018 report from the American Psychological Association, Black people have for years made up the majority of new HIV cases amongst trans people.
Then there’s COVID-19. Per the Williams Institute data, about 217,000 trans people, almost 16 percent of the 1.4 million counted, were over 65. Close to 15 percent had asthma, about double the rate of the general adult population. Higher rates of poverty and homelessness stemming from discrimination against trans people make it harder to shelter in place, noted Kerith Conron, the institute’s research director. Those factors all increase the risk of both contracting COVID-19 and developing complications.
Altogether, the overlapping disparities arguably heighten the need for a vaccine that can be safely recommended for people with HIV, researchers said.
“You wouldn’t want a group excluded for whom we would like to know if the vaccine works,” said Dr. Chris Beyrer, an epidemiologist and AIDS researcher at Johns Hopkins University who is advising enrollment and outreach for Moderna’s clinical trials.
For Mary, the push to include HIV-positive people is valuable. (Mary’s last name has been withheld for privacy reasons.) The lifelong Rhode Islander of Cape Verdean ancestry, has been HIV positive for about 20 years, she said. She takes medication that makes the virus undetectable. Earlier this year, she contracted COVID-19 — she believes it came from being in “close quarters” with other people who had been infected.
Mary recovered after getting plasma and Remsdevir, an experimental treatment, at the local hospital. “It turned my whole situation around,” she said.
She hopes to get a COVID-19 vaccine after one is approved. Moderna’s decision to include HIV positive people in trials “is important,” she said.
There are still questions about other “special populations” who are so far not included in many ongoing vaccine trials. Pregnant people, who research suggests are more vulnerable to complications from COVID-19, are ineligible for Moderna’s and Pfizer’s late-stage trials, according to their records published on ClinicalTrials.gov. Other government-backed vaccine candidates have not posted details about their late-stage trials.
That exclusion, which has drawn attention from federal lawmakers, still has many health researchers concerned. The majority of health care workers are women — within that group, a large percentage are of childbearing age, Swamy noted.
“If they’re not considered at higher risk of disease and don’t get studied in trials they won’t get prioritized at all,” she said. “If we don’t have any safety data on pregnant women, we’re going to be in a tough situation.”
Clarification: This article has been updated throughout to account for differences in data between cisgender and transgender HIV-positive populations.